The primary mechanism of action (MOA) is via serotonin reuptake inhibition, as well as through antagonism of postsynaptic serotonin type two receptors. Trazodone has a variety of mechanisms and is structurally different from other antidepressants. A repeat EKG revealed marked improvement in EKG findings with QTC improving to 485 and QRS narrowing to 102 within two minutes (Figure 3).

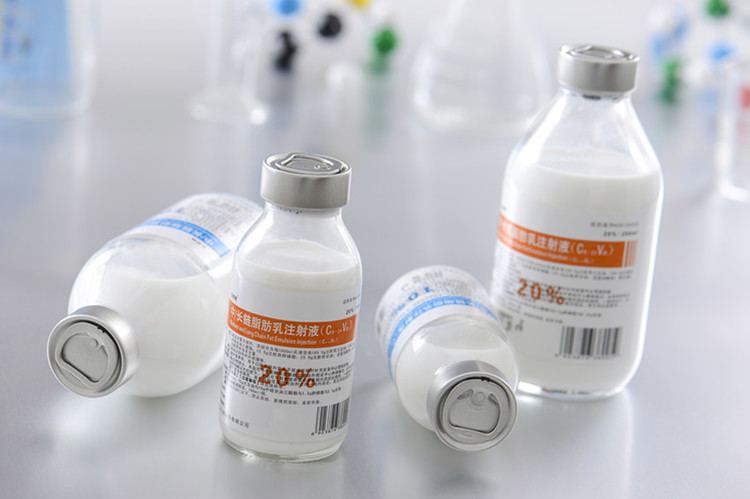
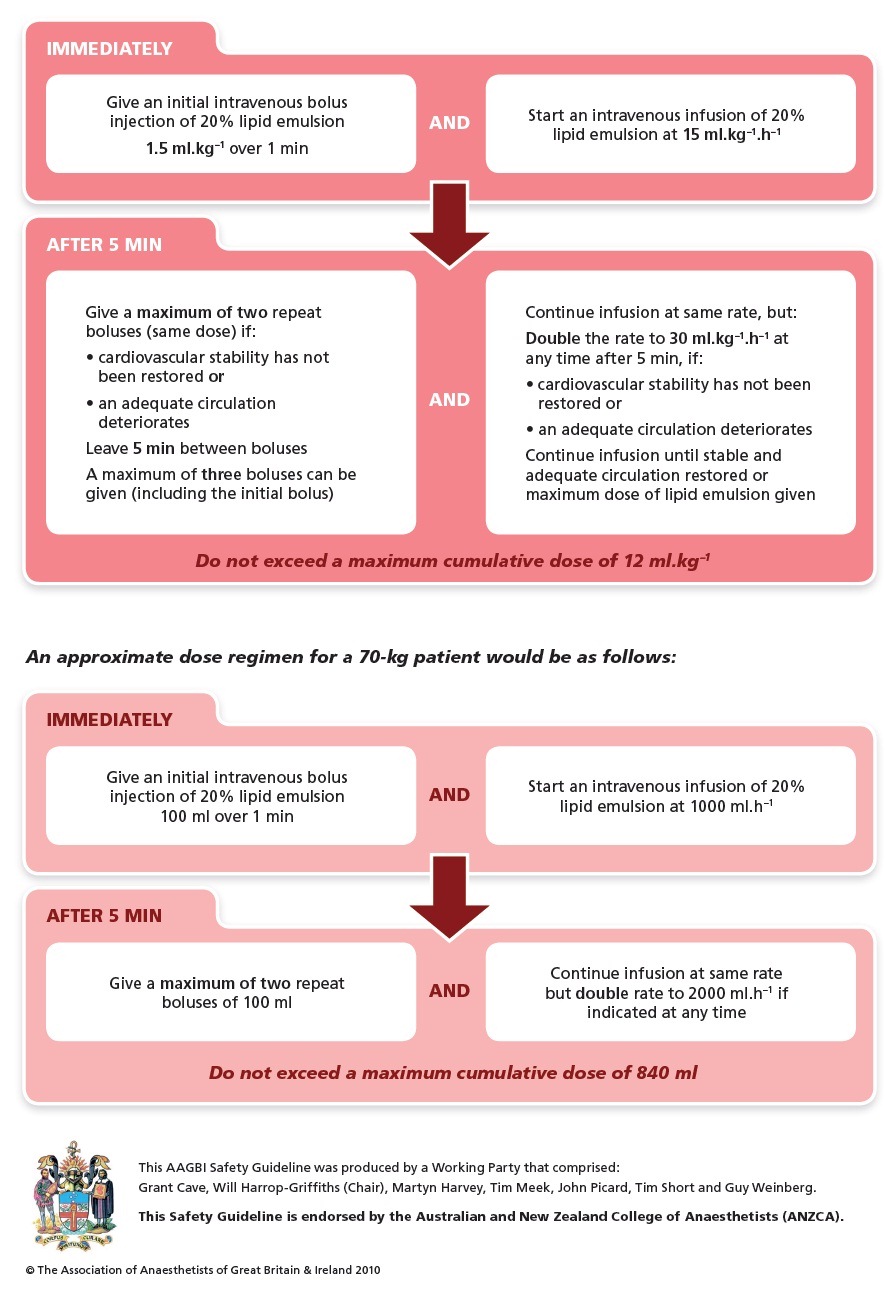
Twenty percent (20%) lipid emulsion was administered as a bolus of 1 mL/kg, and an infusion of 0.25 mL/kg/hr initiated. Return of spontaneous circulation (ROSC) was achieved, and the patient was started on dextrose 5% in water (D5W) plus sodium bicarbonate 150 mEq at 200 mL/hr as well as an amiodarone infusion at 1 mg/min.Īn immediate post-ROSC EKG revealed a prolonged QTC of 539 with widened QRS of 192 (Figure 2). After considering possible sodium channel blockade effect, prolonged QTc, and newly widened QRS complexes, a total of sodium bicarbonate 350 mEq was also given as IV pushes.
The patient received a total of two defibrillation attempts at 200J, epinephrine 1 mg IV, and amiodarone 150 mg IV within a four-minute period. Magnesium sulfate 4 grams intravenously (IV) was immediately administered. Telemetry strips revealed that the patient was in polymorphic ventricular tachycardia (torsades de pointes) just prior to the unresponsive episode. The patient was intubated during this time. The patient suddenly was found to be unresponsive with no palpable pulse. Cardiopulmonary resuscitation (CPR) was immediately started, and advanced cardiac life support (ACLS) protocol followed. However, the patient was noted to have an acute change in clinical status by the one-to-one attendant. The patient was observed in the emergency department for approximately two hours with plans for medical admission. QTc interval was prolonged at 499 milliseconds (Figure 1). Initial EKG showed sinus rhythm at 67 beats per minute with an isolated premature ventricular contraction, narrow QRS with QRS duration noted to be 94 milliseconds. A urine drug screen was negative for opiates, benzodiazepines, marijuana, ecstasy, amphetamines, barbiturates, cocaine, tetrahydrocannabinol, methadone, and phencyclidine. Serum toxicology, including salicylate, acetaminophen, qualitative tricyclic antidepressants (TCA), and ethanol levels, all noted to be undetectable. The thyroid-stimulating hormone level was 1.66 mU/L. VBG was interpreted as chronically stable hypercapnia consistent with the patient's known tobacco use and COPD. Venous blood gas (VBG) performed with pH 7.36, pO2 23 mmHg, pCO2 56 mmHg, bicarbonate 31 mEq/L. Subsequently, oral potassium chloride 40 mEq was given. Chemistry panel was remarkable for sodium 135 mmol/L, potassium 3.0 mmol/L, chloride 97 mmol/L, bicarbonate 33 mmol/L, blood urea nitrogen 11 mg/dL, creatinine 0.8 mg/dL, and glucose 357 mg/dL. Laboratory workup was obtained and revealed a white blood cell count of 3.7, x 10 9/L, hemoglobin 13.8 g/dL, hematocrit 39.7%, and platelets 100 x 10 9/L. Suicide precautions, including one-to-one bedside attendant, were initiated in the emergency department. No specific resuscitative interventions were immediately pursued by the emergency department staff. The physical exam was generally unremarkable. He spoke in clear sentences with no observable neurological deficits on the initial presentation. The patient denied any recreational drug use. His vital signs were within normal limits on arrival: temperature 37.2C, respiratory rate 16, heart rate 92 bpm, blood pressure 126/84 mmHg, and oxygen saturation 100%.
Social history was remarkable for tobacco use, as previously noted as well as social alcohol use. No pertinent family history was reported. Surgical history included a prior lumbar discectomy. He had a prior cardiac catheterization with mild CAD the year prior, and he was treated with medical management. The patient's past medical history was significant for anxiety, depression, coronary artery disease (CAD), congestive heart failure (CHF) with a known left ventricular ejection fraction (LVEF) of 45-50%, chronic obstructive pulmonary disease (COPD), diabetes type II, and tobacco use. The patient had reported taking twenty trazodone 100 mg tablets three hours before arrival. He denied any other coingestants, including alcohol and other illicit drugs. He didn't complain about any symptoms other than feeling slightly fatigued. A 54-year-old male presents to the emergency department via emergency medical services (EMS) after a suicide attempt.
